The discovery, made by Weizmann scientists, could one day help to slow or prevent the disease.
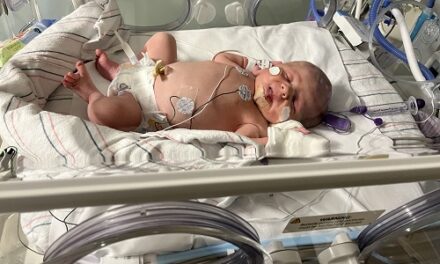
ALS (amyotrophic lateral sclerosis, also known by the name Lou Gehrig’s disease) is a rare – and devastating – neurological disease. Many of us probably didn’t know about it until the Ice Bucket Challenge a few years ago. So what research developments on the disease have been made since then? ALS Awareness Month is a chance to reflect on that and to share a recent discovery at Weizmann that could slow or prevent the disease.
First, we have to understand a little more about ALS itself. One of the reasons it’s such a complicated disease is because it has so many genetic mutations associated with it. There are mutations in over 25 genes associated with ALS, and they all increase the risk of developing it. But now, there appears to be one that decreases that risk.
Weizmann’s Prof. Eran Hornstein and his team have linked a new gene to ALS that contains mutations that play a defensive, rather than an offensive, role in the disease. Let’s start from the beginning to see how it works.
ALS attacks motor neurons, the nerve cells responsible for controlling voluntary muscle movement involved in everything from walking to talking and breathing. The neurons gradually die off, ultimately causing respiratory failure and death. One of the symptoms of ALS is inflammation in the brain regions connected to the dying neurons, caused by immune mechanisms in the brain. If you have a degenerative disease, your brain’s immune cells, called microglia, will try to protect you, attacking the cause of the neurodegeneration.
The problem is that in ALS, the neurodegeneration becomes so severe that the chronic microglial activation in the brain rises to extremely high levels, turning toxic. The immune system thus ends up causing damage to the brain it set out to protect, leading to the death of more motor neurons.
That’s where the new findings, published recently in Nature Neuroscience, come in. This new gene (called IL18RAP) has been long known to affect microglia, and the Weizmann scientists found that it can contain mutations that mitigate the microglia’s toxic effects. “We have identified mutations in this gene that reduce inflammation,” said Dr. Chen Eitan, who led the study in Hornstein’s lab together with Dr. Aviad Siany.
After analyzing the genomes of more than 6,000 ALS patients and of more than 70,000 people who do not have ALS, the researchers concluded that the newly identified mutations reduce the risk of developing ALS nearly fivefold. It is therefore extremely rare for ALS patients to have these protective mutations, and those rare patients who do harbor them tend to develop the disease roughly six years later, on average, than those without the mutations. In other words, the mutations seem to be linked to a core ALS process, slowing the disease down.
To confirm the findings, the researchers used gene-editing technology to introduce the protective mutations into stem cells from patients with ALS, causing these cells to mature into microglia in a laboratory dish. They then cultured microglia, with or without the protective mutations, in the same dishes with motor neurons. Microglia harboring the protective mutations were found to be less aggressive toward motor neurons than microglia that did not have the mutations. “Motor neurons survived significantly longer when cultured with protective microglia, rather than with regular ones,” said Dr. Siany.
Dr. Eitan noted that the findings have potential implications for ALS research and beyond. “We’ve found a new neuroprotective pathway,” she said. “Future studies can check whether modulating this pathway may have a positive effect on patients. On a more general level, our findings indicate that scientists should not ignore noncoding regions of DNA – not just in ALS research, but in studying other diseases with a genetic component as well.”